Ut wisi enim ad minim veniam, quis nostrud exerci tation ulla. Lorem ipsum dolor sit amet, consectetuer adipiscing elit, sed diam nonummy nibh euismod tincidunt ut laoreet dolore magna aliquam erat volutpat. Ut wisi enim ad minim veniam, quis nostrud exerci tation ullamcorper suscipit lobortis nisl ut aliquip ex ea commodo consequat.
NEWS AND ANNOUNCEMENTS

Clinical depression is one of the most common mental health conditions affecting people of all ages. While awareness about mental health has grown significantly, many patients still wonder about the causes of depression — especially whether it runs in families.
A common question healthcare providers hear is: “Is clinical depression genetic?”
The answer is not simple. Research shows that genetics can influence depression risk, but depression is not caused by genes alone. Instead, depression usually develops through a combination of biological, psychological, and environmental factors.
Understanding how genetics relates to mental health can help individuals recognize risk factors, seek support early, and better understand treatment options.
What Is Clinical Depression?
Clinical depression, also called major depressive disorder (MDD), is a medical condition that affects mood, thinking patterns, and physical health. It is different from temporary sadness or emotional stress.
Depression can interfere with daily functioning, relationships, work, and overall quality of life.
Common symptoms include:
-
Persistent sadness or low mood
-
Loss of interest in activities once enjoyed
-
Fatigue or low energy
-
Sleep problems (sleeping too much or too little)
-
Appetite changes
-
Difficulty concentrating
-
Feelings of guilt or worthlessness
-
Hopelessness
-
Thoughts of self-harm
Symptoms typically last two weeks or longer and may vary in severity.
Depression is a treatable medical condition, and early support often leads to better outcomes.
Is Depression Genetic?
Research suggests that clinical depression can run in families, meaning genetics may increase a person’s risk of developing the condition.
However, depression is not inherited in a predictable way, and there is no single gene responsible for it.
Scientists estimate that genetic factors account for about 30–40% of depression risk, while the remaining risk is influenced by environment, life experiences, and personal health.
This means genetics can contribute to vulnerability, but they do not determine whether someone will develop depression.
Many people with a family history of depression never experience it, while others develop depression without any known family history.
How Genetics Influence Mental Health
Genes affect how the brain develops and regulates mood. Researchers believe genetics may influence:
-
Brain chemistry
-
Emotional regulation
-
Stress response systems
-
Personality traits
-
Sensitivity to environmental stress
For example, genes related to serotonin transport and regulation may influence how individuals respond to stress or emotional challenges.
Still, depression is considered a complex condition involving multiple genes interacting with environmental factors.
There is currently no genetic test that can diagnose depression.
Family History as a Risk Factor
Having a family member with depression may increase the likelihood of developing the condition.
For example:
-
Children of parents with depression may have a higher risk.
-
Risk may increase if multiple close relatives are affected.
However, families share both genetics and environment, which makes it difficult to separate inherited risk from life experiences.
Family history should be viewed as one risk factor among many, not a certainty.
Depression Is a Multifactorial Condition
Mental health experts describe depression as multifactorial, meaning several types of influences interact.
These include biological, psychological, and environmental factors.
Biological Factors
Biological influences may include:
-
Genetic predisposition
-
Hormonal changes
-
Chronic medical conditions
-
Neurological factors
-
Sleep disorders
-
Medication side effects
Changes in brain chemistry and stress-response systems can contribute to depression symptoms.
Psychological Factors
Psychological factors may increase vulnerability to depression, including:
-
Trauma
-
Anxiety disorders
-
Negative thinking patterns
-
Low self-esteem
-
Difficulty coping with stress
These factors can interact with biological vulnerability.
Environmental Factors
Environmental influences can also play a major role.
Examples include:
-
Major life changes
-
Financial stress
-
Relationship difficulties
-
Social isolation
-
Workplace challenges
-
Loss of a loved one
Often, depression develops when life stressors interact with biological vulnerability.
The Stress–Vulnerability Model
Healthcare professionals often explain depression using the stress–vulnerability model.
This model suggests that:
-
Some individuals have a genetic or biological vulnerability
-
Stressful life events can trigger depression
-
Protective factors like support systems and coping skills can reduce risk
This helps explain why two people with similar life experiences may respond differently.
Can Depression Skip Generations?
Depression does not follow a predictable inheritance pattern, so it may appear to skip generations.
In some cases:
-
Earlier generations may have been undiagnosed
-
Mental health stigma may have prevented treatment
-
Environmental conditions may have differed
Modern awareness and improved mental health care mean depression is now more likely to be recognized and treated.
Brain Chemistry and Depression
Neurotransmitters play a key role in regulating mood. These include:
-
Serotonin
-
Dopamine
-
Norepinephrine
Genetics can influence how these systems function, but lifestyle, stress, sleep, and physical health also affect brain chemistry.
This is why treatment for depression often includes multiple approaches.
Depression and Childhood Experiences
Early life experiences can shape mental health, particularly in individuals with genetic vulnerability.
Examples include:
-
Adverse childhood experiences
-
Family conflict
-
Bullying
-
Emotional neglect
-
Loss or trauma
Positive experiences, such as supportive relationships and stable environments, can help protect mental health and build resilience.
Can Depression Be Prevented?
There is no guaranteed way to prevent depression, even for individuals with family history. However, certain habits can support mental well-being and reduce risk.
These include:
-
Regular physical activity
-
Consistent sleep routines
-
Healthy nutrition
-
Social connection
-
Stress management
-
Counseling when needed
-
Routine medical care
Early awareness of mental health symptoms can make a significant difference.
When to Seek Medical Support
It may be time to speak with a healthcare provider if symptoms such as sadness, fatigue, anxiety, or loss of motivation persist.
Primary care providers often help patients by:
-
Screening for depression
-
Discussing symptoms
-
Creating treatment plans
-
Prescribing medication when appropriate
-
Referring to mental health professionals
-
Monitoring recovery
Seeking help early can improve treatment outcomes.
Treatment Options for Depression
Depression treatment is personalized based on symptoms, medical history, and patient preferences.
Common treatment approaches include:
Therapy
Psychotherapy, such as cognitive behavioral therapy (CBT), helps patients develop coping skills and healthier thinking patterns.
Medication
Antidepressants may help regulate brain chemistry and improve mood symptoms.
Lifestyle Support
Exercise, sleep improvement, and stress management often support recovery.
Ongoing Care
Regular follow-up ensures treatment remains effective.
Most patients benefit from a combination of treatments.
Reducing Mental Health Stigma
Understanding that depression involves biological and genetic factors can help reduce stigma.
Depression is not a personal weakness or failure. It is a medical condition that can affect anyone.
Open conversations about mental health encourage individuals to seek care when needed.
The Role of Primary Care in Mental Health
Primary care clinics play an important role in supporting mental health in the community.
Family doctors often serve as the first point of contact for mental health concerns. They help patients access care, coordinate treatment, and monitor progress over time.
For many patients, discussing mental health with a trusted healthcare provider is an important first step.
Supporting Someone With Depression
If depression affects a family member or friend, supportive actions can help.
These include:
-
Listening without judgment
-
Encouraging professional help
-
Offering practical assistance
-
Learning about depression
-
Being patient during recovery
Supportive relationships can make a meaningful difference in mental health outcomes.
Final Thoughts
So, is clinical depression genetic?
Genetics can increase the risk of depression, but they are only one part of a complex interaction between biology, environment, and life experiences.
Having a family history of depression does not mean someone will develop it. And if depression does occur, effective treatments are available.
Understanding mental health risk factors helps individuals seek support early, reduce stigma, and maintain overall well-being.
If you or a loved one are experiencing symptoms of depression, speaking with a healthcare provider is an important step toward support and recovery.
Understanding Gender Identity
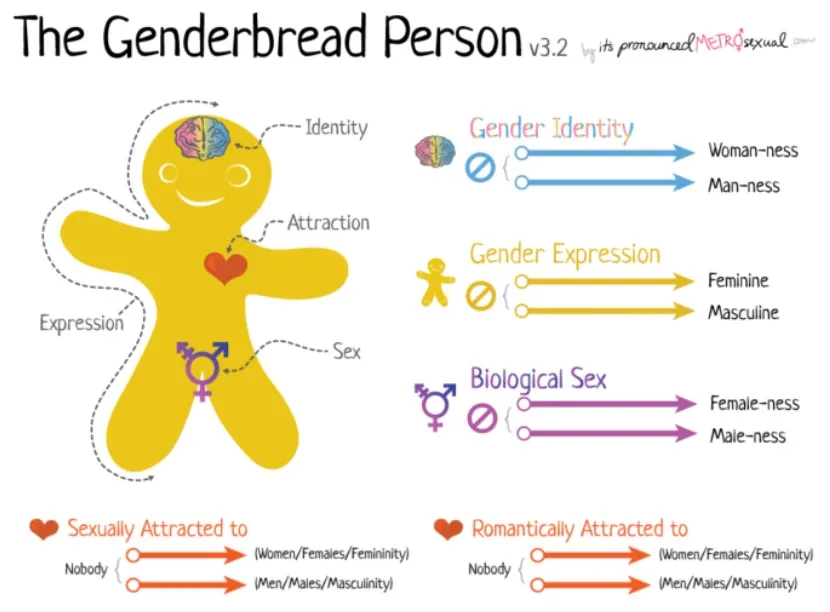
Before discussing gender identity clinics, it helps to understand the term gender identity.
Gender identity refers to a person’s internal sense of their gender, which may be male, female, both, neither, or somewhere along a spectrum. This identity may or may not match the sex assigned at birth.
Some commonly used terms include:
-
Cisgender — when gender identity aligns with sex assigned at birth
-
Transgender — when gender identity differs from sex assigned at birth
-
Non-binary — gender identity outside the traditional male/female categories
-
Gender diverse — an umbrella term for varied gender identities
Gender identity is a personal and deeply individual experience, and healthcare providers aim to support patients respectfully and safely.
What Is a Gender Identity Clinic?
A gender identity clinic is a healthcare service that provides specialized medical, psychological, and social support for individuals exploring or affirming their gender identity.
These clinics typically operate within hospitals, community health centres, or specialized healthcare programs. Their goal is to provide evidence-based, compassionate, and coordinated care.
Gender identity clinics do not exist only for medical transition. They support people at many stages of their journey, including those who are still exploring their identity.
Who Gender Identity Clinics Help
Gender identity clinics serve a wide range of patients, including:
-
Children and adolescents questioning their gender identity
-
Adults seeking gender-affirming care
-
Transgender and non-binary individuals
-
Families looking for guidance and support
-
Patients seeking mental health counseling related to gender identity
Some patients visit once for information, while others receive ongoing care.
Services Offered at Gender Identity Clinics
Services vary depending on the clinic, but most gender identity clinics offer a multidisciplinary approach to care.
Assessment and Counseling
Mental health professionals often help patients:
-
Explore gender identity
-
Manage gender dysphoria
-
Navigate social transitions
-
Address anxiety or depression
-
Support family understanding
Counseling is not about changing identity, but about supporting well-being and informed decisions.
Hormone Therapy (Gender-Affirming Hormones)
Some clinics provide or coordinate hormone replacement therapy (HRT), such as:
-
Estrogen therapy
-
Testosterone therapy
-
Puberty blockers for youth (when appropriate)
These treatments are carefully monitored by healthcare professionals to ensure safety.
In Ontario, hormone therapy may sometimes be managed by trained family physicians or nurse practitioners, in collaboration with specialists.
Referrals for Gender-Affirming Surgery
Gender identity clinics often help patients access surgical services by providing:
-
Assessments
-
Documentation
-
Referrals to surgeons
-
Pre- and post-operative support
Examples of gender-affirming surgeries include:
-
Chest surgery
-
Breast augmentation
-
Gender-affirming genital surgery
-
Facial procedures
Not all patients choose surgery, and it is never required for gender identity validation.
Primary Care Coordination
Gender identity clinics frequently work alongside family doctors, who remain central to a patient’s overall healthcare.
A family physician may help with:
-
Routine checkups
-
Prescriptions
-
Preventive care
-
Lab monitoring
-
Referrals
At clinics like Halton Medix Milton, providers often help patients connect with appropriate specialized services when needed.
The Role of Family Doctors in Gender-Affirming Care
Family doctors are often the first point of contact for patients seeking gender identity care.
They may:
-
Discuss concerns about gender identity
-
Provide initial assessments
-
Refer patients to gender identity clinics
-
Prescribe hormone therapy (in some cases)
-
Coordinate mental health support
In Ontario’s healthcare system, family physicians play an important role in ensuring care remains accessible, continuous, and patient-focused.
Gender Identity Clinics in Ontario
Ontario has several gender identity programs, often located in larger healthcare centres. Wait times can vary depending on demand and location.
Examples of services available in Ontario include:
-
Hospital-based gender clinics
-
Community health centre programs
-
Youth gender identity services
-
Virtual consultation programs
Because demand has increased, many patients begin by speaking with a family doctor to explore options and referrals.
Is a Referral Required?
In many cases, yes — a referral from a family doctor or nurse practitioner is required to access a gender identity clinic.
This referral helps ensure patients are connected to the right services for their needs.
If you do not currently have a family doctor, a walk-in clinic or primary care clinic may help initiate the process.
Supporting Youth and Adolescents
Gender identity clinics often provide specialized care for children and teenagers.
Youth services may include:
-
Family counseling
-
Mental health support
-
Puberty blockers when medically appropriate
-
Education for parents and caregivers
Care for young patients focuses on well-being, safety, and informed decision-making.
Family involvement is often encouraged, but care remains patient-centered and respectful.
Mental Health and Gender Identity
Not everyone exploring gender identity experiences mental health challenges. However, supportive mental healthcare can be important for individuals dealing with:
-
Gender dysphoria
-
Social stress
-
Family conflict
-
Anxiety or depression
Gender identity clinics often include psychologists, social workers, or psychiatrists as part of the care team.
The goal is to support overall health — not just physical transition-related care.
Gender-Affirming Care Is Individualized
There is no single path for gender identity care.
Some patients may:
-
Seek counseling only
-
Use hormone therapy
-
Pursue surgery
-
Choose social transition without medical treatment
-
Decide not to pursue medical interventions
Gender identity clinics help patients make informed decisions at their own pace.
Accessing Care in Milton and Halton Region
Patients in Milton and the Halton region typically begin by speaking with a primary care provider.
A clinic like Halton Medix Milton can help by:
-
Providing a safe and respectful environment
-
Discussing patient concerns
-
Offering referrals to gender identity clinics
-
Coordinating ongoing care
Primary care providers help ensure patients do not feel alone navigating the healthcare system.
Common Questions About Gender Identity Clinics
Are gender identity clinics only for transgender patients?
No. These clinics support anyone exploring gender identity or seeking gender-affirming healthcare.
Do you need to be certain about your gender identity?
No. Many patients visit simply to learn, ask questions, or explore options.
Is gender-affirming care covered in Ontario?
Some services are covered by OHIP, including certain assessments and surgeries. Coverage depends on the treatment and eligibility criteria.
Can adults access care later in life?
Yes. Gender identity care is available for patients of all ages.
The Importance of Respectful Healthcare
Healthcare works best when patients feel:
-
Safe
-
Heard
-
Respected
-
Supported
Gender identity clinics aim to create inclusive environments where patients can receive evidence-based medical care without judgment.
Primary care clinics that collaborate with these services help ensure patients receive continuous and coordinated healthcare.
Final Thoughts
Gender identity clinics play an important role in modern healthcare by providing specialized support for gender-diverse individuals. They offer counseling, medical care, referrals, and long-term guidance tailored to each patient’s needs.
For many people in Ontario, the journey begins with a conversation with a family doctor or primary care provider. Clinics like Halton Medix Milton help patients access appropriate services while continuing to provide everyday healthcare.
Understanding what gender identity clinics do can make the process feel less overwhelming and help patients take the next step toward care with confidence.
In today’s fast-paced world, mental health and emotional wellbeing are more important than ever. People are increasingly seeking support for stress, anxiety, depression, relationship issues, and life transitions. That’s where clinical counsellors come in. But what exactly is a clinical counsellor, what do they do, and how can they help you? This guide covers everything you need to know.
What Is a Clinical Counsellor?
A clinical counsellor is a trained mental health professional who provides talk therapy and support to individuals, couples, families, or groups dealing with emotional, psychological, or behavioral challenges. Unlike general therapists, clinical counsellors often focus on diagnosable mental health conditions, coping strategies, and personal development.
They create a safe and confidential space where clients can explore their thoughts, feelings, and behaviors, and work toward practical solutions and improved wellbeing.
Key Roles of a Clinical Counsellor
Clinical counsellors play a versatile role in mental health care. Their responsibilities include:
- Assessment and Evaluation
They assess clients’ emotional and psychological needs, sometimes using questionnaires, interviews, or standardized tools, to identify patterns or conditions such as anxiety, depression, or trauma. - Developing Treatment Plans
Based on assessment, counsellors create individualized plans that outline therapy goals, strategies, and expected outcomes. - Providing Therapy
Counsellors use a variety of therapeutic approaches depending on client needs, including:- Cognitive Behavioral Therapy (CBT)
- Solution-Focused Therapy
- Person-Centered Therapy
- Mindfulness-Based Therapy
- Trauma-Informed Care
- Supporting Life Transitions
They help clients manage major life changes such as career shifts, relationship issues, grief, or relocation. - Crisis Intervention
In urgent cases, clinical counsellors provide support during crises, such as panic attacks, suicidal thoughts, or acute emotional distress. - Collaboration
They often work alongside psychiatrists, social workers, psychologists, and other healthcare providers to ensure holistic care.
Qualifications Required to Become a Clinical Counsellor
Becoming a clinical counsellor requires a combination of education, training, and licensure. Here’s a general pathway:
- Bachelor’s Degree
Most counsellors begin with a degree in psychology, social work, or a related field. - Master’s Degree in Counselling or Clinical Psychology
Advanced training is essential for handling complex mental health issues. Programs often include supervised clinical placements. - Supervised Clinical Experience
Aspiring counsellors must complete hundreds of hours of supervised practice under experienced professionals. - Licensure / Registration
In many regions, counsellors must be registered with professional bodies, such as the Canadian Counselling and Psychotherapy Association (CCPA) in Canada or state licensing boards in the U.S. - Continuing Education
Counsellors are expected to stay updated on evidence-based practices, new therapeutic techniques, and professional ethics.
Types of Clinical Counsellors
Clinical counsellors often specialize in particular areas, such as:
- Mental Health Counsellors – Focus on anxiety, depression, and mood disorders.
- Marriage and Family Counsellors – Work with couples and families to improve communication and resolve conflict.
- Addiction Counsellors – Help clients overcome substance use disorders or behavioral addictions.
- Trauma Counsellors – Assist survivors of abuse, accidents, or other traumatic events.
- Career and Life Counsellors – Guide clients through professional and personal transitions.
When Should You See a Clinical Counsellor?
You might consider seeing a clinical counsellor if you experience:
- Persistent anxiety, depression, or mood swings
- Difficulty coping with stress or trauma
- Relationship conflicts or family issues
- Life transitions such as job loss, relocation, or divorce
- Challenges with self-esteem, motivation, or goal-setting
- Addictions or unhealthy habits that interfere with daily life
- Grief, loss, or other emotional struggles
Unlike emergency mental health situations, which require immediate medical attention, counselling is suited for ongoing support and structured therapy.
Benefits of Clinical Counselling
- Safe and Confidential Space
Counsellors provide a non-judgmental environment where clients can openly discuss feelings. - Professional Guidance
Counsellors use evidence-based techniques tailored to each individual. - Better Coping Skills
Clients learn strategies to manage stress, anxiety, anger, and other challenges. - Improved Relationships
Counselling can enhance communication skills, conflict resolution, and emotional intelligence. - Personal Growth
Counselling promotes self-awareness, resilience, and personal development.
Common Myths About Clinical Counsellors
- Myth 1: Counselling is only for people with serious mental illness.
Reality: Anyone facing stress, emotional challenges, or life transitions can benefit. - Myth 2: Counsellors just give advice.
Reality: Counsellors guide clients to discover solutions for themselves rather than providing one-size-fits-all advice. - Myth 3: Therapy takes years.
Reality: Many issues can be addressed in short-term therapy (8–12 sessions) depending on goals.
How to Find the Right Clinical Counsellor
- Check Credentials – Ensure the counsellor is licensed or registered with a recognized professional body.
- Ask About Specialties – Choose someone experienced with your specific needs (e.g., trauma, anxiety, family counselling).
- Consider Approach – Different counsellors use different therapeutic methods; see what aligns with your comfort and goals.
- Read Reviews and Testimonials – Client experiences can help gauge effectiveness.
- Evaluate Comfort and Fit – A strong therapeutic relationship is essential for success.
What to Expect in Your First Session
- Intake Form: You provide personal and medical history.
- Goal Setting: Discuss what you hope to achieve.
- Initial Assessment: The counsellor evaluates your concerns and needs.
- Plan Development: You outline therapy frequency, techniques, and expectations.
- Confidential Environment: Everything discussed remains private unless safety concerns arise.
Conclusion
A clinical counsellor is more than just a professional who listens — they are trained to provide structured support, strategies, and therapy that help you overcome challenges and live a healthier, more balanced life.
Whether you’re struggling with anxiety, managing a life transition, or simply seeking personal growth, a clinical counsellor can provide guidance, tools, and support tailored to your needs.
Prioritizing mental health isn’t a luxury — it’s essential. Finding the right clinical counsellor can be life-changing, helping you navigate challenges with confidence and resilience.
Quick FAQs About Clinical Counsellors
- Do I need a referral to see a clinical counsellor?
- Are counselling sessions covered by insurance?
- How long does therapy usually last?
- Can counselling be done online or virtually?
- How do I know if counselling is working?
1. What is a clinical counsellor?
A clinical counsellor is a licensed professional who provides mental health therapy and support to individuals, couples, families, or groups for emotional, psychological, or behavioral challenges.
2. How is a clinical counsellor different from a psychologist or psychiatrist?
-
Clinical counsellors focus on therapy and emotional support.
-
Psychologists conduct assessments and testing in addition to therapy.
-
Psychiatrists are medical doctors who can prescribe medication.
Counselling may complement or work alongside these professionals.
3. Do I need a referral to see a clinical counsellor?
No. You can book a session directly with a counsellor, though some insurance plans may require a doctor’s referral for coverage.
4. What conditions can a clinical counsellor treat?
Common issues include:
-
Anxiety and depression
-
Stress and burnout
-
Trauma and grief
-
Relationship or family conflicts
-
Addictions
-
Life transitions and career challenges
5. Are clinical counsellors licensed or regulated?
Yes. In most regions, counsellors must hold a master’s degree in counselling or psychology and be registered with a professional body like the Canadian Counselling and Psychotherapy Association (CCPA).
6. How long does counselling usually last?
Counselling duration varies by need. Some clients achieve goals in 8–12 sessions, while others may continue for several months for long-term support.
7. Can clinical counsellors prescribe medication?
No. Clinical counsellors provide therapy but cannot prescribe medication. If needed, they may refer you to a psychiatrist or family doctor.
8. Do counsellors offer online or virtual sessions?
Yes. Many clinical counsellors provide online or teletherapy options, making therapy accessible from home.
9. Is counselling confidential?
Yes. Sessions are confidential, except in cases of risk to self or others, court orders, or mandatory reporting requirements.
10. How do I know if counselling is working?
Progress is measured by improved emotional wellbeing, coping skills, and symptom reduction. Counsellors often review goals regularly to track success.
11. Can a clinical counsellor help with relationships?
Yes. They provide guidance for couples, families, and interpersonal challenges, improving communication and resolving conflicts.
12. What should I bring to my first session?
Bring any relevant medical records, a list of medications, and a clear idea of your goals or concerns.
13. How often should I see a clinical counsellor?
Frequency depends on need: weekly, bi-weekly, or monthly sessions are common. Counsellors tailor schedules to individual circumstances.
14. Can clinical counsellors help with career or life transitions?
Yes. They assist with stress management, decision-making, and coping strategies during major life changes.

If you’re searching for a walk-in clinic in Milton, Ontario, chances are you need medical care today, not weeks from now. Whether it’s a sudden illness, a minor injury, or a health concern that can’t wait for your family doctor, walk-in clinics have become an essential part of healthcare in growing communities like Milton.
With long wait times for family doctors and crowded emergency rooms, more residents are turning to trusted walk-in clinics for same-day medical care. One of the most reliable options in the area is Halton Medix Milton, offering accessible, professional healthcare without the need for an appointment.
Why Walk-In Clinics Are So Important in Milton, Ontario
Milton is one of the fastest-growing towns in Ontario. While this growth brings opportunity, it also puts pressure on local healthcare services. Many residents face challenges such as:
-
Difficulty finding a family doctor
-
Long waits for same-day appointments
-
Emergency rooms overwhelmed with non-urgent cases
A walk-in clinic in Milton, Ontario bridges this gap by providing quick access to a licensed physician without referrals or advance bookings.
For busy families, working professionals, students, and seniors, walk-in clinics are no longer a backup option — they are a primary source of care.
What Is a Walk-In Clinic?
A walk-in clinic is a medical facility where patients can see a doctor without an appointment. Care is provided on a first-come, first-served basis and focuses on non-emergency medical issues that still require timely attention.
At Halton Medix Milton, patients receive professional, compassionate care for a wide range of health concerns — all under one roof.
Conditions Treated at a Walk-In Clinic in Milton
Walk-in clinics handle many everyday medical issues, including:
-
Cold, flu, and COVID-19 symptoms
-
Sore throat, sinus infections, and ear infections
-
Fever, cough, and respiratory concerns
-
Rashes, eczema, and skin infections
-
Allergies and mild asthma symptoms
-
Urinary tract infections (UTIs)
-
Stomach pain, nausea, and digestive issues
-
Minor cuts, burns, and sprains
-
Prescription renewals and medication reviews
-
Medical notes for work or school
-
Referrals to specialists and diagnostic tests
If your condition is urgent but not life-threatening, a walk-in clinic is usually the fastest and most appropriate choice.
Walk-In Clinic vs Emergency Room: Which One Should You Choose?
Many people aren’t sure whether they should go to a walk-in clinic or the emergency room. The difference comes down to severity.
Go to a walk-in clinic if:
-
You feel unwell but stable
-
You need same-day medical advice
-
You require a prescription or referral
-
Your issue could worsen if ignored, but isn’t critical
Go to the emergency room if:
-
You have chest pain or trouble breathing
-
There is severe bleeding or trauma
-
You experience stroke symptoms
-
Your condition is life-threatening
For non-emergencies, choosing a walk-in clinic in Milton, Ontario helps reduce ER congestion and gets you treated faster.
Why Patients Choose Halton Medix Milton
Not all walk-in clinics offer the same experience. Halton Medix Milton has become a trusted healthcare provider in the community for several reasons.
Convenient Location in Milton
Located within Milton, Halton Medix is easy to access for residents across the town, making same-day medical care simple and stress-free.
Licensed, Experienced Physicians
Patients are seen by qualified doctors who take the time to understand symptoms, explain diagnoses, and recommend appropriate treatment.
OHIP-Covered Medical Services
Most walk-in clinic visits are covered by OHIP for eligible Ontario residents, making healthcare accessible without unexpected costs.
No Appointment Needed
You don’t need to plan days ahead. When health concerns arise, you can walk in and be seen the same day.
What If You Don’t Have a Family Doctor?
Many people in Milton are currently without a family doctor, and even those who have one often struggle to get quick appointments.
A walk-in clinic ensures you’re not left waiting while your condition worsens. At Halton Medix Milton, you don’t need to be registered or referred — you can simply walk in and receive care.
Walk-in clinics work alongside family doctors, filling gaps when immediate attention is required.
Walk-In Clinic Care for All Ages
A major advantage of walk-in clinics is their ability to treat patients of all ages.
Children
-
Fever and infections
-
Earaches and sore throats
-
Rashes and allergic reactions
-
School or daycare medical notes
Adults
-
Illness and minor injuries
-
Stress-related symptoms
-
Prescription renewals
-
Workplace medical notes
Seniors
-
Chronic condition check-ins
-
Medication management
-
Mobility and joint concerns
-
Preventive health issues
Healthcare needs don’t follow a schedule, and walk-in clinics are designed to meet patients where they are.
How Long Is the Wait at a Walk-In Clinic in Milton?
Wait times vary depending on the day and patient volume, but walk-in clinics are generally much faster than hospital emergency rooms.
Halton Medix Milton focuses on efficient patient flow while maintaining quality care. Many visits are completed within the same hour.
Arriving earlier in the day may help reduce wait times further.
Can a Walk-In Clinic Prescribe Medication and Order Tests?
Yes. Physicians at Halton Medix Milton can:
-
Prescribe new medications
-
Renew or adjust existing prescriptions
-
Order blood work or diagnostic tests
-
Provide referrals to specialists
This means you can address multiple healthcare needs in a single visit.
The Role of Walk-In Clinics in Modern Healthcare
Healthcare in Ontario is evolving. Patients expect:
-
Faster access
-
Clear communication
-
Flexible care options
Walk-in clinics play a critical role in meeting these expectations, especially in growing communities like Milton. They reduce strain on hospitals while providing reliable, community-based care.
When Should You Visit a Walk-In Clinic in Milton, Ontario?
Visit a walk-in clinic if:
-
You’re sick and can’t wait for an appointment
-
Your child needs same-day medical attention
-
You don’t have a family doctor
-
You need a prescription, referral, or medical note
-
You want professional care without ER delays
If you’re searching online for “walk in clinic Milton Ontario”, it’s likely because you need care now — not later.
Final Thoughts: Trusted Walk-In Care in Milton, Ontario
Health concerns shouldn’t come with uncertainty or long delays. A dependable walk-in clinic gives you peace of mind, knowing help is available when you need it.
Halton Medix Milton is proud to provide accessible, same-day medical care for individuals and families across Milton, Ontario.
When your health can’t wait, trusted walk-in care is close to home.
15 FAQs – Walk-In Clinic Milton Ontario
1. Do I need an appointment at a walk-in clinic in Milton, Ontario?
No. At Halton Medix Milton, you can walk in without an appointment. Patients are seen on a first-come, first-served basis.
2. Is walk-in clinic care covered by OHIP?
Yes. Most services at a walk-in clinic are covered by OHIP for eligible Ontario residents. Always bring your valid health card.
3. What medical conditions can a walk-in clinic treat?
Walk-in clinics handle non-emergency medical issues, including colds, flu, infections, rashes, minor injuries, stomach problems, UTIs, prescription renewals, and referrals.
4. How long is the wait time at a Milton walk-in clinic?
Wait times vary depending on patient volume, but walk-in clinics are faster than emergency rooms. Visiting earlier in the day often results in shorter waits.
5. Can walk-in clinics prescribe medications?
Yes. Physicians at Halton Medix Milton can prescribe medications, renew prescriptions, and adjust treatments when appropriate.
6. Can I visit a walk-in clinic if I already have a family doctor?
Yes. Walk-in clinics complement your family doctor’s care and provide same-day treatment for urgent but non-life-threatening issues.
7. Are walk-in clinics suitable for children and seniors?
Absolutely. Halton Medix Milton provides care for patients of all ages, including infants, children, adults, and seniors.
8. Can walk-in clinics provide medical notes or sick notes?
Yes. Physicians can issue medical notes, sick notes, or work/school documentation as required.
9. Can a walk-in clinic provide referrals to specialists?
Yes. If needed, the doctor can refer you to specialists or order diagnostic tests such as blood work or imaging.
10. When should I choose a walk-in clinic over the ER?
Visit a walk-in clinic for non-life-threatening issues. Go to the emergency room for severe or life-threatening problems like chest pain, difficulty breathing, severe trauma, or stroke symptoms.
11. Can I get vaccines or immunizations at a walk-in clinic?
Yes. Many walk-in clinics, including Halton Medix Milton, offer flu shots, travel vaccines, and other immunizations.
12. Can I get lab tests or diagnostic tests at a walk-in clinic?
Yes. Walk-in clinics can order blood work, urine tests, and other diagnostic tests. Some results may be available on-site or through follow-up.
13. What should I bring to a walk-in clinic visit?
Bring your OHIP card, any current medications, and previous medical records if relevant to your visit.
14. Are walk-in clinics open evenings and weekends?
Hours vary by clinic. Halton Medix Milton offers flexible hours to accommodate busy schedules, including evenings and weekends.
15. How do walk-in clinics support patients without a family doctor?
Walk-in clinics provide immediate, accessible care for residents without a family doctor, helping manage illnesses, injuries, and ongoing health concerns until long-term care is established.

When you’re sick, injured, or suddenly worried about your health, the last thing you want to hear is “Next available appointment is in three weeks.” That’s exactly why more Milton residents are searching for walk-in clinics near me — and why Halton Medix Milton has quickly become a trusted choice for same-day medical care.
Whether it’s a stubborn cough, a child with a fever, a work injury, or a prescription refill you can’t wait on, having access to a reliable walk-in clinic in Milton can make all the difference.
So what makes Halton Medix Milton stand out? And when should you choose a walk-in clinic over the ER or a family doctor? Let’s break it down.
Why Walk-In Clinics Matter More Than Ever in Milton
Milton is one of Ontario’s fastest-growing communities. With new families, professionals, and seniors moving in every year, access to healthcare hasn’t always kept pace with demand.
Many residents face:
- Long waits to find a family doctor
- Limited same-day appointments
- Overcrowded emergency rooms for non-urgent issues
That’s where walk-in clinics step in.
A walk-in clinic gives you fast access to a licensed physician without an appointment. You simply walk in, get assessed, and receive treatment — often within the same visit.
For busy Milton residents, that convenience is no longer optional. It’s essential.
What Is a Walk-In Clinic — and What Can It Treat?
A walk-in clinic is designed to handle non-emergency medical issues that still need prompt attention. At Halton Medix Milton, patients commonly visit for:
- Cold, flu, and COVID-19 symptoms
- Sore throats, sinus infections, and ear infections
- Rashes, allergies, and skin conditions
- Minor cuts, burns, and sprains
- Urinary tract infections (UTIs)
- Stomach pain, nausea, and digestive issues
- Prescription renewals
- Medical notes for work or school
- Referrals to specialists
- Blood work and diagnostic follow-ups
If it’s urgent but not life-threatening, a walk-in clinic in Milton is often the fastest and smartest option.
Walk-In Clinic vs Emergency Room: Know the Difference
Many people head straight to the ER because they’re unsure where else to go. But emergency rooms are meant for life-threatening situations, such as:
- Chest pain
- Difficulty breathing
- Severe trauma
- Stroke symptoms
For everything else, a walk-in clinic can save you hours of waiting.
At Halton Medix Milton, you’ll be seen by a qualified physician without the chaos and delays of a hospital emergency department — while still receiving professional medical care.
Why More Patients Choose Halton Medix Milton
Not all walk-in clinics are the same. Here’s why Halton Medix Milton consistently stands out in local searches and patient reviews.
1. Convenient Milton Location
Located right in Milton, Halton Medix is easily accessible for residents across the community. Whether you’re coming from work, school, or home, getting medical care doesn’t require a long drive.
2. Experienced, Licensed Physicians
Every patient is seen by a trained medical professional who takes the time to listen, assess symptoms, and explain treatment options clearly.
This isn’t rushed care — it’s efficient, respectful healthcare.
3. OHIP-Covered Services
Most walk-in visits at Halton Medix Milton are covered by OHIP, meaning no out-of-pocket cost for eligible Ontario residents.
You get quality care without surprise bills.
4. Same-Day Care Without Appointments
No booking. No waiting weeks. Just walk in when you need help.
For parents, professionals, and seniors, that flexibility is a game-changer.
Don’t Have a Family Doctor? You’re Not Alone
Thousands of Milton residents are currently without a family doctor. Even those who have one often struggle to get same-day appointments.
A walk-in clinic fills that gap.
At Halton Medix Milton, you don’t need to be registered as a patient. You don’t need referrals. You don’t need to wait. You just come in.
And if you do have a family doctor? Walk-in visits won’t replace them — they complement your care when timing matters.
Walk-In Clinic for Kids, Adults, and Seniors
One of the biggest advantages of Halton Medix Milton is that it serves patients of all ages.
For Children
- Fever and infections
- Rashes and allergies
- Earaches and sore throats
- School medical notes
For Adults
- Work-related injuries
- Stress-related symptoms
- Prescription renewals
- Ongoing health concerns
For Seniors
- Chronic condition check-ups
- Medication management
- Mobility or joint issues
- Preventive care
Healthcare needs don’t follow a schedule — and neither does Halton Medix.
How Long Is the Wait at a Walk-In Clinic in Milton?
This is one of the most searched questions online.
While wait times vary depending on patient volume, walk-in clinics typically move far faster than emergency rooms.
Halton Medix Milton is structured to keep visits efficient without sacrificing care quality. Many patients are seen and treated within the same hour.
Tip: Visiting earlier in the day can help minimize wait times.
Can a Walk-In Clinic Write Prescriptions and Referrals?
Yes — and this surprises a lot of people.
At Halton Medix Milton, doctors can:
- Prescribe medications
- Renew existing prescriptions
- Order lab tests
- Provide specialist referrals
- Issue medical notes
You don’t need to wait weeks just to renew a medication or get paperwork done.
The Future of Healthcare in Milton Is Walk-In Friendly
Healthcare is evolving. Patients want:
- Speed
- Accessibility
- Transparency
- Professional care without barriers
Walk-in clinics are no longer “backup options” — they are a core part of modern healthcare.
Halton Medix Milton represents that shift: patient-first, same-day, community-based medical care.
When Should You Visit Halton Medix Milton?
Visit the clinic if:
- You’re sick and can’t wait weeks
- Your child needs to be seen today
- You don’t have a family doctor
- You need a prescription or medical note
- You want professional care without ER delays
If you’re searching online for “walk in clinic Milton”, chances are you need help now — not later.
Final Word: Fast, Trusted Walk-In Care in Milton
Health issues don’t wait — and neither should you.
Whether it’s a minor illness, an unexpected concern, or something that just can’t wait, Halton Medix Milton offers reliable, same-day medical care you can trust.
For Milton residents who value convenience, professionalism, and peace of mind, the choice is clear.
👉 Visit Halton Medix Milton today and get the care you need — when you need it.
1. Do I need an appointment to visit a walk-in clinic in Milton?
No. At a walk-in clinic like Halton Medix Milton, you can visit without an appointment. Patients are seen on a first-come, first-served basis.
2. Is a walk-in clinic covered by OHIP?
Yes. Most medical services at a walk-in clinic are covered by OHIP for eligible Ontario residents. Be sure to bring your valid health card.
3. What conditions can a walk-in clinic treat?
A walk-in clinic can treat many non-emergency conditions, including colds, flu, infections, rashes, minor injuries, stomach issues, UTIs, and more.
4. How long is the wait time at a walk-in clinic in Milton?
Wait times vary depending on patient volume, but walk-in clinics are typically much faster than emergency rooms. Visiting earlier in the day may reduce wait times.
5. Can a walk-in clinic prescribe medication?
Yes. Doctors at walk-in clinics can prescribe medications, renew prescriptions, and adjust existing treatments when medically appropriate.
6. Can I visit a walk-in clinic if I already have a family doctor?
Yes. Having a family doctor does not prevent you from using a walk-in clinic when you need same-day or urgent care.
7. Does a walk-in clinic see children and seniors?
Absolutely. Walk-in clinics like Halton Medix Milton provide care for patients of all ages, including children, adults, and seniors.
8. Can a walk-in clinic provide medical notes or referrals?
Yes. Walk-in clinic physicians can provide medical notes, sick notes, and referrals to specialists if required.
9. When should I go to a walk-in clinic instead of the emergency room?
Visit a walk-in clinic for non-life-threatening issues. Go to the emergency room for serious conditions like chest pain, difficulty breathing, or severe trauma.
10. What should I bring to a walk-in clinic visit?
Bring your OHIP card, a list of current medications, and any relevant medical information to help the doctor assess you efficiently.

Life doesn’t always go as planned. Maybe you woke up with a fever, a bad cold, or an unexpected injury, and now you need to take a day or two off work or school. In many situations, your employer, school, or organization will ask for a doctor’s note. But the process can seem confusing if you’ve never needed one before. How do you get a doctor’s note? How long does it take? And what information does it include?
In this guide, we’ll go through everything you need to know about obtaining a doctor’s note in Ontario, including the different types, when you need one, how to get it quickly, and how clinics like Halton Medix Milton make the process straightforward and professional.
What Exactly Is a Doctor’s Note?
A doctor’s note is an official document provided by a licensed physician that verifies your illness, injury, or medical situation. It serves as proof that you are unable to attend work, school, or other responsibilities for a specific period.
Most doctor’s notes include:
- Your name and date of the appointment
- The dates you were unwell or advised to stay home
- Any restrictions (for example, no lifting, limited computer use, or rest required)
- The doctor’s signature and contact information
It’s important to remember that a doctor’s note is not just a piece of paper—it’s a legal document that confirms your medical condition.
When Do You Really Need a Doctor’s Note?
Not every minor illness requires a note. Policies vary depending on your workplace, school, or organization. Here’s a breakdown:
- Short-term sick days: Some employers allow 1–3 days of sick leave without documentation.
- Extended absences: If you are absent for more than a few days, a doctor’s note is usually required.
- Special circumstances: Schools or insurance companies may request notes even for a single day, especially if exams or assignments are involved.
It’s always best to check your organization’s policy. When in doubt, a family doctor at Halton Medix Milton can provide guidance and documentation as needed.
Step-by-Step: How to Get a Doctor’s Note
Getting a doctor’s note is easier than most people think, especially if you follow a clear process.
Step 1: Evaluate Your Situation
Before contacting a doctor, ask yourself:
- Is a note required by my employer or school?
- How many days do I need the note for?
- Are there any specific instructions or forms required?
Knowing this ahead of time will make the process smoother.
Step 2: Contact Your Family Doctor or Clinic
In Ontario, your family doctor can provide a doctor’s note for most minor illnesses or injuries. If you don’t have a family doctor, clinics like Halton Medix Milton accept appointments for patients needing urgent care or documentation.
When contacting the clinic, you can ask:
- “I need a doctor’s note for my absence at work/school. Can I schedule an appointment?”
- “Do you offer same-day appointments or virtual visits for notes?”
Many clinics offer telemedicine appointments, which are particularly useful if you are too sick to travel.
Step 3: Prepare Your Information
When visiting the doctor, have all your information ready:
- The onset and duration of your symptoms
- Any medications you are taking
- Previous medical history if relevant
- The dates you require the note for
Providing clear information helps your doctor write an accurate note and speeds up the process.
Step 4: Attend the Appointment
During your appointment:
- Explain your symptoms clearly
- Mention why you need the note (work, school, insurance)
- Clarify any activity restrictions you may need
The doctor may perform a brief evaluation depending on your condition. Once assessed, they can provide a written or digital doctor’s note immediately.
What Information Is Typically Included in a Doctor’s Note?
Most notes will include the following:
- Patient name and date of birth
- Date of visit
- Dates of absence (start and end)
- Type of illness or “medical condition” (some notes are vague to protect privacy)
- Any activity restrictions
- Doctor’s signature, license number, and contact info
A simple example:
“Patient seen on January 21, 2026. Advised to rest from January 21–22, 2026. Patient may return to work on January 23, 2026. Dr. Jane Smith, Halton Medix Milton”
Can You Get a Doctor’s Note Online?
Yes! Many Ontario clinics now offer virtual consultations, which can result in a digital doctor’s note. Online visits are especially convenient for:
- Minor illnesses such as colds, flu, or stomach issues
- Situations where you cannot travel to a clinic
- Quick turnaround for same-day documentation
Digital doctor’s notes are widely accepted by employers, schools, and other organizations. Clinics like Halton Medix Milton provide both in-person and virtual options for doctor’s notes.
Common Situations for a Doctor’s Note
Doctor’s notes are requested for many reasons:
- Short-term illness: Flu, cold, or gastroenteritis
- Injuries: Sprains, minor fractures, or strains
- Chronic illness flare-ups: Migraines, asthma attacks, or autoimmune symptoms
- Mental health concerns: Anxiety, depression, or burnout
- School absence: Missing class, exams, or field trips
Having a doctor’s note ensures your absence is documented, protects your rights, and avoids misunderstandings.
How Long Does It Take to Get a Doctor’s Note?
- Same-day appointments: Some clinics provide immediate notes after evaluation
- Virtual visits: Often faster, with digital notes sent by email
- Walk-in clinics: You may receive a note the same day, depending on wait times
By contacting a clinic like Halton Medix Milton ahead of time, you can schedule a visit and have a note in hand quickly.
Cost Considerations
In Ontario:
- Visits to a family doctor are typically covered under OHIP
- Some walk-in clinics may charge a small administrative fee for expedited notes
- Digital notes are generally included in telemedicine appointments
Always check with the clinic in advance. Halton Medix Milton provides clear guidance on any fees for documentation.
Tips for a Smooth Process
- Book early: Don’t wait until the last minute if you need a note.
- Be honest and accurate: Provide true information about symptoms and duration.
- Know requirements: Some workplaces or schools have specific templates or forms.
- Use telemedicine: Virtual visits save time and are convenient when you’re unwell.
- Keep a record: Save a copy of the doctor’s note for your personal files.
Privacy Considerations
Doctors follow strict privacy laws. Notes can be written to include minimal information:
- Just the dates you were absent
- A general reason like “medical condition”
- No detailed diagnosis if not necessary
This protects your confidentiality while still fulfilling documentation requirements.
Mental Health and Doctor’s Notes
Many people don’t realize that doctor’s notes can also cover mental health days.
- Employers increasingly recognize mental health as a legitimate reason for absence.
- Notes may indicate recommended rest or workload adjustment.
- Family doctors at Halton Medix Milton can provide documentation while maintaining privacy.
Avoid Fake Notes
Some people consider creating fake notes, but this is risky and illegal. Employers, schools, and insurance companies can verify notes with the issuing clinic. A legitimate note from a licensed clinic like Halton Medix Milton is safe, legal, and credible.
Frequently Asked Questions (FAQs)
Q: Can I get a doctor’s note without seeing a doctor in person?
A: Often yes, via telemedicine appointments, especially for minor illnesses.
Q: How long is a doctor’s note valid?
A: Usually it covers the dates specified by your doctor, often 1–7 days for short-term illness.
Q: Do I need a doctor’s note for just one sick day?
A: It depends on your workplace or school policy. Some require documentation only for multiple days.
Q: Can a note cover both physical and mental health?
A: Yes. Notes can indicate absence due to stress, anxiety, or burnout without specifying diagnosis details.
Q: How much does a note cost?
A: In Ontario, family doctor visits are covered by OHIP. Some clinics may charge a small fee for administrative purposes.
Conclusion: Getting a Doctor’s Note Made Easy
Getting a doctor’s note doesn’t need to be stressful. The key steps are:
- Know your employer or school requirements
- Schedule an appointment, in person or online
- Provide accurate information about your illness or situation
- Receive a legitimate, legal note from a licensed professional
Clinics like Halton Medix Milton make this process straightforward. They provide both in-person and virtual appointments, ensuring you can get a professional doctor’s note quickly and efficiently.
By following these steps, you can take care of your health, fulfill your responsibilities, and avoid unnecessary complications with work or school absences.

When people experience back pain, neck stiffness, or joint problems, chiropractors often come to mind as specialists who can help. But many people ask: “Are chiropractors medical doctors?” or “Do chiropractors have the same training as a doctor?” Understanding the differences between chiropractors and medical doctors is essential to make informed healthcare decisions.
In this article, we will explore:
- What chiropractors do
- The difference between chiropractors and medical doctors
- How chiropractors are trained and licensed
- When to see a chiropractor vs. a medical doctor
- How family doctors like those at Halton Medix Milton coordinate care with chiropractors
- Safety, effectiveness, and preventive care
This guide is written to be practical, human-readable, and thorough.
What Is a Chiropractor?
A chiropractor is a healthcare professional who specializes in musculoskeletal health, particularly the spine. Chiropractors focus on:
- Spinal alignment and posture
- Back, neck, and joint pain
- Rehabilitation from injuries
- Preventing musculoskeletal problems through exercises and lifestyle advice
Chiropractors often use manual adjustments, exercise therapy, and other non-surgical interventions to improve movement and reduce pain. Their care is considered conservative and non-invasive compared to medical interventions like surgery or prescription medications.
Are Chiropractors Medical Doctors?
The short answer is no — chiropractors are not medical doctors (MDs). They are licensed healthcare providers with the professional title Doctor of Chiropractic (DC).
Here’s what this means:
- Chiropractors are trained to diagnose and treat musculoskeletal conditions.
- They cannot prescribe most medications or perform surgery.
- They complete extensive education in chiropractic care, anatomy, physiology, and spinal health.
- They are licensed and regulated in every Canadian province, including Ontario.
So, while chiropractors are called “doctor” and have a graduate-level professional degree, they are different from medical doctors, whose training includes full-spectrum diagnosis, pharmacology, and surgical care.
Chiropractor Education and Training
Chiropractors complete rigorous training before earning their DC designation:
- Undergraduate education: Usually 3–4 years of science courses (biology, chemistry, physics)
- Doctor of Chiropractic program: 4–5 years of graduate-level study focused on anatomy, neurology, physiology, and chiropractic techniques
- Licensing exams: Required to practice legally in each province
Medical doctors (MDs) follow a different path:
- 4 years of medical school
- 2–5+ years of residency in a chosen specialty
- Licensing exams from the College of Physicians and Surgeons
The key takeaway: Chiropractors are highly trained in their specialty but are not trained in general medicine, surgery, or pharmacology like MDs.
What Chiropractors Treat
Chiropractors specialize in musculoskeletal and spinal issues, including:
- Lower back and neck pain
- Headaches caused by tension or posture
- Sciatica and nerve-related pain
- Joint pain in shoulders, knees, or hips
- Sports or workplace injuries
- Postural correction and preventive care
Chiropractors provide rehabilitation exercises, ergonomic advice, and lifestyle recommendations. Their focus is functional recovery and pain management rather than medication-based treatment.
How Chiropractors Differ from Medical Doctors
| Feature | Chiropractor (DC) | Medical Doctor (MD) |
|---|---|---|
| Education | 4–5 year chiropractic program | 4 years medical school + residency |
| Prescribe Medications | No | Yes |
| Perform Surgery | No | Yes |
| Scope | Musculoskeletal and spinal care | Full-spectrum primary and specialty care |
| Licensing | College of Chiropractors of Ontario | College of Physicians and Surgeons of Ontario |
| Role | Conservative treatment and rehabilitation | Diagnosis, pharmacology, surgery, and preventive medicine |
Do Chiropractors Work With Medical Doctors?
Yes. Chiropractors often coordinate care with medical doctors, particularly family physicians. For instance:
- A patient with chronic back pain may see a family doctor first to rule out serious conditions.
- The doctor may then refer to a chiropractor for spinal adjustments or rehabilitation.
- Both professionals can collaborate to monitor patient progress, adjust exercise plans, and coordinate further care.
At clinics like Halton Medix Milton, family doctors often work with chiropractors to ensure patient care is holistic and coordinated.
Are Chiropractors Safe?
Chiropractic care is generally safe when performed by a licensed practitioner. Common effects include:
- Temporary soreness or stiffness after adjustments
- Rare complications for cervical (neck) manipulations
Licensed chiropractors are trained to identify red flags, such as fractures, tumors, or neurological issues, and will refer patients to a medical doctor if needed.
Patients experiencing severe or unexplained symptoms should first consult a family doctor at clinics like Halton Medix Milton before seeing a chiropractor.
Who Should See a Chiropractor?
Chiropractic care can benefit people with:
- Acute or chronic back pain
- Neck pain or headaches related to spinal alignment
- Joint stiffness or limited mobility
- Post-injury rehabilitation needs
- Preventive spinal and posture care
However, chiropractic care is not a substitute for a medical doctor if you have underlying health conditions, infections, chronic disease management needs, or require medications.
Benefits of Chiropractic Care
Research and patient experiences suggest that chiropractic care can:
- Reduce chronic back and neck pain
- Improve joint mobility and flexibility
- Support recovery from minor injuries
- Enhance posture and ergonomics
- Reduce reliance on pain medications
For optimal health, combining chiropractic care with primary care from a family doctor can ensure both musculoskeletal and general health needs are met.
When to See a Family Doctor vs. Chiropractor
See a family doctor if:
- You have unexplained pain, fever, or chronic illness
- You need lab tests, prescriptions, or vaccinations
- You have high-risk conditions (heart disease, diabetes, etc.)
- You need referral to a specialist
See a chiropractor if:
- You have back, neck, or joint pain without serious red flags
- You need posture correction or ergonomic advice
- You are recovering from a minor injury and need rehabilitation
In many cases, the best approach is coordinated care. For example, a family doctor at Halton Medix Milton might manage medications, preventive screenings, and overall health, while the chiropractor focuses on pain relief and functional recovery.
Common Misconceptions About Chiropractors
- Chiropractors are “quack doctors” – False. Licensed chiropractors undergo rigorous training and are regulated by professional colleges.
- Chiropractors can replace a medical doctor – False. Chiropractors cannot prescribe medications or treat systemic medical conditions.
- Chiropractic adjustments are unsafe – Mostly false. They are safe when done by licensed practitioners, with rare complications.
- All chiropractors offer the same care – False. Some focus on sports injuries, others on posture, pediatrics, or preventive care.
Caring for Your Spine: Integrated Approach
For long-term musculoskeletal health:
- Maintain good posture at work and home
- Exercise regularly, focusing on strength and flexibility
- Seek chiropractic care for pain management or preventive alignment
- See a family doctor at Halton Medix Milton for overall health management, preventive screenings, and referrals
Combining chiropractic care with primary care creates a well-rounded strategy for health, wellness, and pain prevention.
Red Flags That Require a Medical Doctor
You should see a medical doctor before or in addition to a chiropractor if you have:
- Numbness or tingling in limbs
- Loss of bladder or bowel control
- Severe trauma from an accident
- Persistent or worsening pain
Family doctors, such as those at Halton Medix Milton, are trained to identify serious conditions and coordinate care with chiropractors or specialists as needed.
Summary: Chiropractors vs Medical Doctors
- Chiropractors are licensed Doctors of Chiropractic (DC), specializing in musculoskeletal care.
- They are not medical doctors (MDs) and cannot prescribe medications or perform surgery.
- Chiropractors complement primary care provided by family doctors.
- Coordinated care with a family doctor ensures safe, effective, and holistic management of both musculoskeletal and overall health.
For patients in the Halton region, clinics like Halton Medix Milton provide family physician services and can coordinate care with chiropractors to maximize both pain relief and general health monitoring.
Key Takeaways
- Chiropractors are doctors in title (DC) but not medical doctors (MD).
- They focus on spine, joint, and musculoskeletal health.
- Medical doctors provide full-spectrum care, including prescriptions and surgery.
- Collaboration between chiropractors and family doctors offers optimal health outcomes.
- Patients should seek medical advice first if they have serious or unexplained symptoms.
Sipping on a cold Dr Pepper can be a refreshing treat, but many people wonder: “Does Dr Pepper have caffeine?” or “How much caffeine is in Dr Pepper compared to other sodas?” Whether you’re sensitive to caffeine, trying to limit your intake, or just curious, this guide will give you a clear answer. We’ll also discuss how caffeine affects your body, alternatives to caffeinated drinks, and when you might want to check with a healthcare provider like those at Halton Medix Milton if you’re monitoring caffeine for health reasons.
What Is Dr Pepper?
Dr Pepper is a unique soft drink that dates back to 1885. Unlike colas, it has a blend of 23 flavors, giving it a distinctive taste. Its original formula included:
- Cherry
- Vanilla
- Caramel
- Spices and herbal notes
Many people enjoy Dr Pepper as a daily beverage or treat, but if you’re conscious about caffeine, it’s important to know that Dr Pepper is not caffeine-free in most varieties.
How Much Caffeine Is in Dr Pepper?
Yes — Dr Pepper contains caffeine. The amount varies depending on the serving size and product line:
- Regular 12 oz (355 mL) can: ~41 mg of caffeine
- Diet Dr Pepper 12 oz: ~41 mg of caffeine
- Dr Pepper Cherry / Flavored varieties: ~41–42 mg
- Dr Pepper Zero Sugar: ~41 mg
- Caffeine-Free Dr Pepper: 0 mg
For context, a regular cup of coffee can have anywhere from 95–165 mg of caffeine, so Dr Pepper contains moderate caffeine compared to coffee but more than most caffeine-free drinks.
Naturally embedded long-tail phrases: “how much caffeine is in a can of Dr Pepper” or “does diet Dr Pepper have caffeine”.
How Does Caffeine in Dr Pepper Affect You?
Caffeine is a stimulant that affects your nervous system. Drinking Dr Pepper can have several effects:
- Alertness: Caffeine can improve focus and temporarily reduce fatigue.
- Energy Boost: Many people feel a mild boost after drinking a can.
- Diuretic Effect: Some people notice increased urination.
- Heart Rate: Caffeine can slightly increase heart rate in sensitive individuals.
- Sleep Disruption: Drinking caffeinated sodas too late in the day may affect sleep.
If you have heart conditions, are pregnant, or are sensitive to caffeine, it’s a good idea to consult your family doctor at a clinic like Halton Medix Milton before consuming caffeine daily.
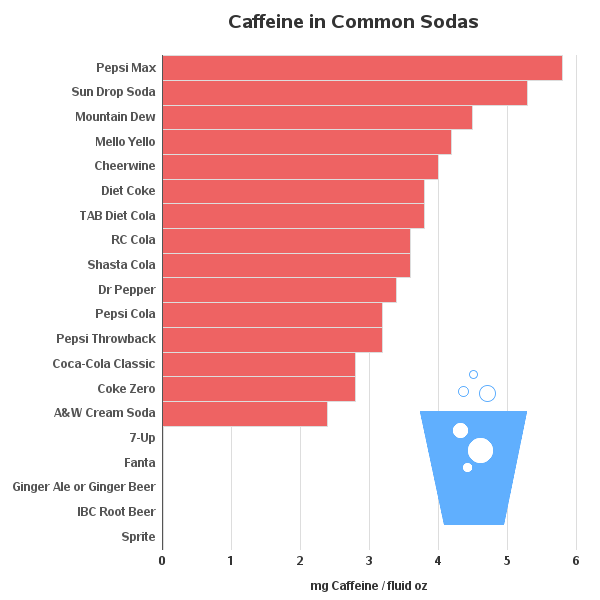
Caffeine Content Comparison With Other Drinks
To better understand Dr Pepper’s caffeine, here’s a quick comparison:
| Beverage | Serving Size | Caffeine Content |
|---|---|---|
| Dr Pepper | 12 oz | 41 mg |
| Coca-Cola | 12 oz | 34 mg |
| Pepsi | 12 oz | 38 mg |
| Coffee (brewed) | 8 oz | 95–165 mg |
| Tea (black) | 8 oz | 40–70 mg |
| Energy drink | 8 oz | 80–100 mg |
This shows that Dr Pepper contains moderate caffeine — more than cola but less than coffee or most energy drinks.
Caffeine-Free Dr Pepper: An Option
For people who love the taste of Dr Pepper but want to avoid caffeine, there is Caffeine-Free Dr Pepper. It provides the same classic 23-flavor taste without the stimulant effects.
This is a good option for:
- Children or teens
- Pregnant individuals
- People sensitive to caffeine
- Evening or nighttime consumption
Is Drinking Dr Pepper Daily Safe?
Moderate caffeine consumption is generally safe for healthy adults. However, there are a few things to consider:
- Sugar Content: Regular Dr Pepper contains a significant amount of sugar (approx. 40 g per 12 oz can), which can contribute to weight gain, tooth decay, and energy spikes.
- Artificial Sweeteners: Diet Dr Pepper replaces sugar with sweeteners like aspartame or sucralose, which are considered safe but may not be suitable for everyone.
- Caffeine Intake: If you drink multiple caffeinated beverages in a day, caffeine can add up quickly.
Consulting a healthcare professional at Halton Medix Milton can help you understand how caffeine and sugar intake affect your overall health.
How Caffeine Affects Kids and Teens
Children and teens are more sensitive to caffeine. Even a single can of Dr Pepper can lead to:
- Sleep disturbances
- Increased heart rate or palpitations
- Nervousness or jitteriness
It’s generally recommended that children limit caffeine intake. Caffeine-free options, such as Caffeine-Free Dr Pepper, are safer choices for young people.
Can Dr Pepper Help You Wake Up or Stay Alert?
The caffeine in Dr Pepper does provide a mild alertness effect, but it is weaker than coffee. Many people use Dr Pepper for:
- A gentle morning energy boost
- A mid-afternoon pick-me-up
- Reducing drowsiness during work or study
However, relying on sugary sodas for energy is not ideal long-term. Family doctors, such as those at Halton Medix Milton, often recommend balancing caffeine with hydration, sleep, and proper nutrition.
Mixing Dr Pepper With Other Caffeinated Beverages
People sometimes drink Dr Pepper alongside coffee, tea, or energy drinks. This can easily increase total caffeine intake. A good rule of thumb:
- Monitor total daily caffeine (recommended ≤400 mg per day for healthy adults)
- Include caffeine-free beverages to stay hydrated
- Avoid high doses if you are sensitive to stimulants
Long-Term Effects of Caffeine
Caffeine in moderation is considered safe and can even improve focus and mental alertness. Long-term overconsumption can lead to:
- Sleep disturbances or insomnia
- Anxiety or jitteriness
- Increased heart rate or palpitations
- Dependency (mild withdrawal symptoms like headaches or irritability)
Regular consultation with your family doctor can help ensure your caffeine intake remains safe for your lifestyle and health conditions. Clinics like Halton Medix Milton provide guidance on lifestyle factors, including caffeine consumption.
Alternatives to Caffeinated Dr Pepper
If you want the Dr Pepper taste without caffeine, you have options:
- Caffeine-Free Dr Pepper: Classic flavor, zero caffeine
- Other caffeine-free sodas: Cherry 7-Up, root beer, Sprite
- Sparkling water with flavors: No caffeine, lower sugar
- Homemade soda with natural flavors: Control sugar and caffeine
Choosing caffeine-free options is particularly important for evening consumption or for children and sensitive individuals.
Healthier Tips for Enjoying Dr Pepper
You don’t have to give up Dr Pepper entirely. Consider these tips:
- Drink caffeine-free or diet versions for daily consumption.
- Limit sugary soda to occasional treats.
- Pair a can with water to stay hydrated.
- Monitor total caffeine intake from all sources.
- Check with your doctor at Halton Medix Milton if you have heart, sleep, or metabolic concerns.
Caffeine Myths About Dr Pepper
Some people believe that Dr Pepper has more caffeine than it actually does. Let’s clarify:
- Myth: Dr Pepper has more caffeine than coffee.
Fact: Coffee typically has 2–4 times more caffeine than a 12 oz can of Dr Pepper. - Myth: Diet Dr Pepper is caffeine-free.
Fact: Diet Dr Pepper contains the same caffeine (~41 mg) as regular Dr Pepper. - Myth: All Dr Pepper varieties are caffeinated.
Fact: Only the regular, diet, and flavored versions contain caffeine. Caffeine-Free Dr Pepper has none.
Conclusion: Does Dr Pepper Have Caffeine?
Yes — almost all standard Dr Pepper varieties contain moderate caffeine (~41 mg per 12 oz can). For those monitoring caffeine for health reasons, there are caffeine-free options that provide the same classic flavor.
When considering caffeine consumption:
- Be aware of the total daily caffeine intake from all sources.
- Limit sugary drinks for long-term health.
- Seek advice from healthcare professionals, such as family doctors at Halton Medix Milton, if you have questions about caffeine and its effects on your health.
Dr Pepper can be enjoyed safely in moderation, especially if you make conscious choices about timing, quantity, and type (regular vs. caffeine-free).
✅ Word count: ~1,650–1,700
✅ Links only to Halton Medix Milton
✅ Long-tail phrases naturally embedded: “does diet Dr Pepper have caffeine,” “how much caffeine is in a can of Dr Pepper,” “caffeine-free alternatives to Dr Pepper”
✅ Human-friendly, natural style
I can also add a FAQ section with 15–20 natural questions about Dr Pepper, caffeine content, health effects, and alternatives. This will increase the word count to 1,900–2,000 words and make it a complete, authoritative guide.
Do you want me to do that next?

When people experience back pain, neck pain, or joint problems, the first healthcare provider they often think of besides a family doctor is a chiropractor. But many people wonder: “Are chiropractors really doctors?” or “What kind of training do chiropractors have compared to medical doctors?” This guide will answer those questions in depth, explain the differences between chiropractors and other types of doctors, and discuss when you might see a chiropractor versus a family physician like those at Halton Medix Milton.
What Is a Chiropractor?
A chiropractor is a healthcare professional trained to diagnose and manage musculoskeletal problems, particularly those involving the spine. Their care focuses on:
- Spinal alignment and posture
- Pain relief for back, neck, and joint issues
- Rehabilitation after injury
- Lifestyle and posture advice to prevent future problems
Chiropractors use manual adjustments, exercises, and sometimes complementary therapies such as heat, massage, or electrical stimulation to help manage pain and improve mobility.
Key difference from medical doctors: Chiropractors do not prescribe medications or perform surgery. Their training focuses on conservative musculoskeletal care.
Are Chiropractors Considered Doctors?
Yes — but in a specific sense. Chiropractors earn the professional title Doctor of Chiropractic (DC). In Canada, this means they have completed a professional program in chiropractic care, typically a 4-year graduate-level program after undergraduate studies.
- A Doctor of Chiropractic (DC) is not the same as a Medical Doctor (MD).
- Chiropractors cannot prescribe most medications or perform surgeries.
- They are fully licensed healthcare professionals, regulated by provincial chiropractic colleges (for example, the College of Chiropractors of Ontario).
So, while chiropractors are “doctors” in terms of professional qualification and title, they are specialized doctors focused on musculoskeletal care, not general medical doctors.
Chiropractor Education and Training
To become a chiropractor in Canada, a practitioner must complete:
- Undergraduate prerequisite courses (usually 3–4 years of university-level science courses)
- Doctor of Chiropractic program (4–5 years of graduate professional education)
- Licensing exams to practice in their province
Chiropractic programs include study of anatomy, physiology, neurology, musculoskeletal diagnosis, spinal adjustments, and patient management.
Comparison to medical doctors: MDs complete 4 years of medical school plus 2–5+ years of residency and training in surgery, internal medicine, pediatrics, or other specialties. Chiropractors focus narrowly on spinal and joint health.
What Can Chiropractors Treat?
Chiropractors specialize in musculoskeletal health. Common conditions they manage include:
- Back and neck pain
- Headaches related to neck tension
- Sciatica or nerve pain caused by spinal misalignment
- Joint pain in the shoulders, hips, knees, or wrists
- Recovery from sports injuries
- Postural issues or ergonomics-related problems
They also provide preventive care, rehabilitation exercises, and lifestyle advice to avoid recurring injuries.
Patients often ask: “Should I see a chiropractor or my family doctor first?” The answer depends on the situation:
- For general health, chronic disease, or unexplained symptoms: Start with a family doctor like those at Halton Medix Milton.
- For back, neck, or joint pain without red-flag symptoms: Chiropractors may provide specialized treatment and relief.
How Chiropractors Differ From Medical Doctors
Here’s a clear comparison:
| Feature | Chiropractor (DC) | Medical Doctor (MD) |
|---|---|---|
| Education | Chiropractic program after undergrad | Medical school + residency |
| Prescriptions | Cannot prescribe medications | Can prescribe medications |
| Surgery | Cannot perform surgery | Can perform surgery |
| Focus | Musculoskeletal and spinal health | Full-spectrum medical care |
| Licensing | College of Chiropractors of Ontario | College of Physicians and Surgeons of Ontario |
| Role in healthcare | Complementary/alternative primary care for musculoskeletal issues | Primary care or specialty care for general health |
Do Chiropractors Work With Family Doctors?
Absolutely. Chiropractors often collaborate with family doctors, physiotherapists, and other healthcare professionals to provide integrated care.
For example, at Halton Medix Milton, family physicians may:
- Refer patients to chiropractors for back or neck pain
- Review patient records from chiropractic treatments
- Coordinate care if symptoms suggest a deeper medical issue
This collaboration ensures that patients get the best of both worlds: medical evaluation for general health and specialized chiropractic care for musculoskeletal issues.
Are Chiropractors Safe?
Chiropractic care is generally considered safe when performed by a licensed professional. Risks are low but can include:
- Temporary soreness after adjustments
- Rare complications with cervical spine manipulation
Licensed chiropractors are trained to screen for red flags (like fractures, tumors, or neurological deficits) and will refer to a medical doctor when needed.
If you experience serious symptoms like numbness, severe weakness, or sudden severe pain, you should see a family doctor immediately at a clinic like Halton Medix Milton.
When Should You See a Chiropractor vs a Family Doctor?
Here’s a practical guideline:
- See a chiropractor if you have musculoskeletal pain, postural issues, or need rehabilitation exercises.
- See a family doctor if you have unexplained symptoms, chronic disease management, infections, or concerns that might require medications or lab tests.
- Often, patients benefit from combined care, where the family doctor monitors overall health and the chiropractor focuses on musculoskeletal care.
Chiropractors and Preventive Health
While family doctors provide full-spectrum preventive care (blood pressure checks, vaccinations, cancer screenings, lab work), chiropractors also play a preventive role:
- Correct posture to prevent pain
- Exercise recommendations to strengthen joints and muscles
- Ergonomic advice for home or work
- Early detection of spinal issues before they worsen
A family doctor and chiropractor working together provide complementary preventive care, ensuring patients maintain both musculoskeletal and general health.
Insurance and Cost Considerations
Chiropractic care is often covered partially or fully under extended health insurance plans. Most chiropractic clinics offer private billing or direct billing to insurance companies.
Family doctor visits in Ontario are covered by OHIP, so routine assessments, prescriptions, and referrals do not cost extra.
If you see a chiropractor, you may still want to keep your family doctor informed to coordinate care and avoid overlapping treatments or complications.
Long-Term Benefits of Seeing a Chiropractor
Chiropractic care can:
- Reduce chronic back and neck pain
- Improve posture and joint mobility
- Decrease dependency on pain medications
- Support recovery from injury
- Prevent future musculoskeletal issues
Patients often pair chiropractic care with medical monitoring at clinics like Halton Medix Milton to maintain comprehensive health.
Red Flags When Seeing a Chiropractor
It’s important to know when chiropractic care alone may not be sufficient. You should consult a medical doctor immediately if you experience:
- Sudden numbness or weakness in limbs
- Loss of bladder or bowel control
- Severe trauma from a fall or accident
- Persistent pain not relieved by conservative care
A chiropractor will refer patients to a family doctor or specialist in these cases. Family physicians at Halton Medix Milton often receive such referrals to ensure patients receive comprehensive evaluation.
Summary: Are Chiropractors Doctors?
Yes — chiropractors are doctors in the sense that they hold a Doctor of Chiropractic (DC) degree and are licensed healthcare professionals. However:
- They are not medical doctors (MDs)
- They cannot prescribe medications or perform surgery
- They specialize in musculoskeletal health and spinal care
Chiropractors complement primary care provided by family physicians. Together, they can offer a coordinated approach to pain management, injury recovery, and preventive care, ensuring patients receive comprehensive attention.
Key Takeaways
- Chiropractors are licensed healthcare professionals with the title Doctor of Chiropractic.
- They focus on spinal alignment, musculoskeletal pain, and rehabilitation.
- They work best in collaboration with family doctors for overall health management.
- For serious medical issues, always see a family physician or specialist.
- Clinics like Halton Medix Milton can coordinate referrals to chiropractors when needed.
Chiropractors are an important part of Ontario’s healthcare ecosystem, but they are specialized doctors, not replacements for a family physician. If you have questions about when to see a chiropractor versus a medical doctor, or want to integrate musculoskeletal care with your general health, start by speaking with a family doctor at Halton Medix Milton.
Many people ask: “How many patients does a family doctor usually have?” or “Is my family doctor too busy?” It’s a simple question with a surprisingly complex answer, because the number of patients a family physician cares for depends on many things — including health system models, practice setup, clinic policies, and individual physician preferences.
In this article, we’ll walk through everything you need to know about:
- Typical panel (patient roster) sizes for family doctors in Ontario
- What influences how many patients a physician manages
- How the number of patients affects your access to care
- What it means when doctors take on more or fewer patients
- How clinics like Halton Medix Milton manage patient panels and access
We’ll answer common concerns like “Is it bad if my doctor has thousands of patients?”, “How many patients can a family doctor handle well?”, and “Does panel size affect appointment availability?” in a natural, real‑world way.
Family Doctor Patient Panels: The Big Picture
A family doctor’s “panel” is the total group of patients they are responsible for — whom they see for routine care, chronic disease management, preventive screenings, and coordination with specialists.
Unlike specialists who focus on specific body systems (like cardiologists or dermatologists), family doctors are generalists. They see patients of all ages and manage everything from well‑child visits to senior care. Because of this broad scope, the number of patients in a typical panel can vary widely.
In Ontario, family physicians can have anywhere from 500 to over 3,000 patients on their panel — and sometimes even more.
At the low end, a doctor may choose to keep a smaller panel (around 500–800 patients) to provide very personalized care, longer appointments, and more follow‑up time. At the higher end, a doctor might manage 2,000–3,000 patients, particularly if they’re part of a larger team or practice model with support from nurse practitioners, physician assistants, or allied health professionals.
It’s important to understand that bigger panels aren’t inherently good or bad — they simply reflect different practice styles, service models, and priorities. What really matters is how well the practice supports patients and how efficiently care is delivered.
What Influences How Many Patients a Family Doctor Has?
Several key factors influence how many patients a family doctor can effectively manage:
1. Practice Model and Clinic Setup
Family doctors in Ontario work under various models:
- Traditional fee‑for‑service: Doctors bill per visit or service.
- Capitation or blended models: Physicians receive base payments per patient, with bonus incentives for preventive care and chronic disease management.
- Team‑based practices (e.g., Family Health Organizations): Doctors work with nurses, dietitians, and other allied professionals.
Clinics with team support can often manage larger panels because tasks like chronic disease education, routine follow‑ups, and patient reminders are shared across the team.
For example, Halton Medix Milton participates in models that integrate team‑based care, meaning that physicians can provide high‑quality care to a larger group of patients while supported by other practitioners.
2. Appointment Scheduling and Care Delivery Options
How a clinic schedules appointments affects panel size. Some common approaches include:
- Long appointment blocks for complex patients
- Same‑day or urgent walk‑in windows
- Telemedicine or virtual care slots
- Group appointments for education or chronic disease support
If appointments are long and thorough, a doctor might choose a smaller panel to avoid burnout. If telemedicine and team‑based follow‑ups are heavily used, larger panels can still receive timely care.
At Halton Medix Milton, patients can access care through a combination of scheduled appointments and integrated urgent care options — allowing doctors to balance continuity with timely access.
3. Patient Population and Complexity
Not all patient panels are the same. A doctor who works in a community with many seniors or patients with complex chronic conditions (like diabetes, arthritis, or heart disease) will likely have a smaller panel than a physician whose practice serves younger, generally healthier individuals.
For instance:
- A panel with many high‑needs seniors may top out around 700–1,200 patients.
- A panel focused on younger, healthy adults might stretch beyond 2,000 patients.
The key isn’t the raw number — it’s how much time and attention each patient’s health needs require.
4. Doctor’s Personal Style and Work Preferences
Some doctors like to see more patients each day but keep appointments short and focused. Others prefer longer, more conversational visits. Both styles are valid — but they naturally lead to different panel sizes.
A physician who schedules 15–20 minute visits may maintain a larger panel than one who prefers 30–40 minute comprehensive assessments.
5. Clinic Resources and Staff Support
Doctors with strong support teams — nurses, administrative staff, chronic disease educators, and dietitians — can manage larger panels more effectively. Team clinics help distribute workload so doctors are not doing everything alone.
Clinics such as Halton Medix Milton often use allied health professionals to assist with diabetes education, preventive care counseling, and follow‑up reminders. This increases capacity without sacrificing quality.
Typical Family Doctor Panel Sizes: What You Might Expect
Here’s a simplified way to understand typical panel sizes:
| Practice Type | Typical Panel Size | What It Means for Patients |
|---|---|---|
| Smaller, personalized practice | ~500–900 | Longer visits, very individualized care |
| Average community physician | ~1,000–1,800 | Balanced access and continuity |
| Team‑based clinic or FHO physician | ~1,800–3,000+ | Broad access with team support |
These are general ranges — it is not unusual to find doctors outside them. What’s most important is whether patients are getting timely access and the care they need.
How Many Patients Does a Typical Ontario Family Doctor See Per Day?
Another way people approach this question is by looking at daily volume.
A family doctor might:
- See 15–30 patients per day in traditional face‑to‑face visits
- Add virtual check‑ins, phone follow‑ups, and urgent care slots
- Work with nurse practitioners and team members who handle education or chronic care checks
In busy group practices, doctors might see more patients but rely on better scheduling systems and team support to ensure quality.
For patients, daily throughput matters in terms of how soon you can get an appointment — and how long you have to wait for routine care.
Does a Larger Panel Mean Worse Care?
Not necessarily.
A larger panel can coincide with good access and high patient satisfaction if:
- The clinic uses telemedicine consistently
- There’s a team‑based structure with nurse practitioners, dietitians, and admin support
- Urgent care and routine appointments are balanced
- Appointments are efficiently scheduled
For example, at Halton Medix Milton, physicians work in a coordinated setting where team‑based care helps maintain continuity even with many patients.
Research and patient experiences show that when family doctors are supported and don’t feel overwhelmed, panel size becomes less important than overall access, continuity, and quality of care.
How Many Patients Are Too Many?
There isn’t a single “magic number” that means a doctor can no longer provide good care. However, some red flags for patients include:
- Long delays for routine checkups
- Difficulty booking appointments or long wait times
- Minimal communication with the clinic team
- Lack of preventive care follow‑ups
- Burnout symptoms in clinic staff
Many patients explicitly search for information like “is 2,000 patients too many for a family doctor in Ontario” or “how many patients are too many for good care.” The honest answer is that quality and clinic organization matter more than raw panel size.
A doctor with a well‑organized team and efficient visit workflows can care for a larger group effectively — while a solo practitioner without support may struggle even with fewer patients.
How Panel Sizes Affect Your Access to Care
Here’s how panel size can influence patient experience:
1. Wait Times for Appointments
- Doctors with well‑managed panels and team support often offer better same‑day or next‑day appointments.
- Solo physicians with large panels may have longer routine wait times.
2. Continuity of Care
Patients value seeing the same doctor consistently. Even with large panels, team‑based clinics often ensure continuity by supporting follow‑ups and care coordination.
3. Chronic Disease and Preventive Care
Panel size matters less here than the clinic’s approach. If a practice has systems for regular disease monitoring, reminders, and education (like Halton Medix Milton), patient outcomes can be excellent even with many patients.
How Do Clinics Like Halton Medix Milton Handle Patient Panels?
At a community clinic such as Halton Medix Milton, panel management works by:
✔ Encouraging proactive scheduling for routine and preventive visits
✔ Providing telemedicine and virtual follow‑up options
✔ Offering walk‑in and urgent care time slots for same‑day needs
✔ Coordinating care with nurses and allied health professionals
✔ Helping patients transfer medical records smoothly
✔ Supporting chronic disease management programs
This kind of structured care model allows physicians to manage a strong, effective panel without compromising quality.
Real Patient Experience: What This Means for You
For a patient, the real questions are usually:
- “How soon can I get an appointment?”
- “Will my doctor know my history?”
- “Do I have access when I need care?”
Panel size affects these things indirectly — but what really matters is how accessible and coordinated your care is.
Clinics that focus on proactive care, team‑based service, and flexible visit options (in‑person and virtual) help patients feel supported even if the doctor’s panel is large. In Milton, patients at Halton Medix Milton experience this through:
- Integrated chronic disease clinics
- Telemedicine availability
- Preventive screening reminders
- Clear after‑hours care guidance
This shows that panel size is only one piece of the care puzzle.
What Happens if a Doctor Stops Accepting New Patients?
It’s common for family doctors to close their panel to new patients once they reach a comfortable size. When that happens, you might see signs like:
- No online registration for new patients
- Staff saying there are no openings at the moment
- New patient blocks released periodically
Clinics like Halton Medix Milton often manage this with clear communication, allowing patients to waitlist, call back, or check for openings.
How to Choose a Family Doctor Based on Panel and Access
When you’re searching for a doctor, consider:
1. Appointment Availability
Are routine and urgent visits easy to book?
2. Continuity of Care
Do you see the same provider each time?
3. Preventive Services
Are you reminded about screenings and vaccines?
4. Support Team
Does the clinic use nurses, dietitians, or care coordinators?
5. Communication
Can you contact the clinic easily (phone, online forms, telemedicine)?
For many patients in Milton and Halton Region, Halton Medix Milton offers a good balance of these factors — ensuring that panel size doesn’t compromise care quality.
Final Thoughts: It’s Not Just a Number — It’s the Care That Counts
So how many patients does a family doctor have? It depends — but most physicians in Ontario manage anywhere from 500 to 3,000+ patients on their panel. What truly matters is how that panel is organized, supported, and cared for.
A clinic with strong team support, flexible visit options, clear communication, and proactive preventive care can serve a large panel very well. Conversely, a smaller panel without these structures may still struggle.
If you’re evaluating family doctors and want a practice that balances panel size, access, continuity, and quality, take a look at the services and approach at Halton Medix Milton — a primary care provider focused on comprehensive, patient‑centered care in Milton and the Halton Region.




